Update on the management of COPD | Lesson
A 60 year old man presents to his GP in May 2013 complaining of shortness of breath on exertion and recurrent chest infections.
The GP ascertains that the patient has been breathless and wheezy for about 4 years and gets about 3 episodes of bronchitis a year for which he doesn’t usually receive any treatment. During infections he produces about a tablespoon of purulent sputum daily but normally produces very little sputum.
His current exercise tolerance is only 100 yards on the flat and he rarely exercises anymore. He has smoked since the age of 15 with an average of 30 per day and has never tried to quit. He worked as a carpenter but had to quit two years previously due to breathlessness. He has a history of hypertension and hypercholesterolaemia and drinks about 30 units of alcohol per week.
On examination he has a BMI of 35 and is not distressed at rest. He has no anaemia, finger clubbing or central cyanosis and oxygen saturation on room air is 95%. He is hyperinflated with decreased air entry bilaterally and diffuse expiratory wheeze. He has no evidence of right heart failure. His leg muscles appear wasted.
The GP suspects COPD and performs spirometry 20 mins after inhaling 200µg of salbutamol through a spacer. The FEV1/FVC ratio is decreased at 60% and the FEV1 is 55% predicted and the FVC 80% predicted confirming moderate GOLD SPIROMETRY stage 2 COPD (see Table 1).
The GP proceeds to fully stage the patient according to the latest GOLD 2013 guidelines (see Table 2). CAT score (see Table 4) was 18.
The patient is initially staged according to the horizontal axis by mMRC graded exercise tolerance (Table 3) and CAT questionnaire (Table 4) score to determine how symptomatic his disease is. The patient’s MMRC of 3 and CAT score of 18 initially places the patient in symptomatic group B. The table is then read vertically to incorporate risk of future exacerbations. The FEV1 is GOLD stage 2 but he is a high frequency exacerbator at 3 per year (see Table 5) placing him finally in the most severe group D.
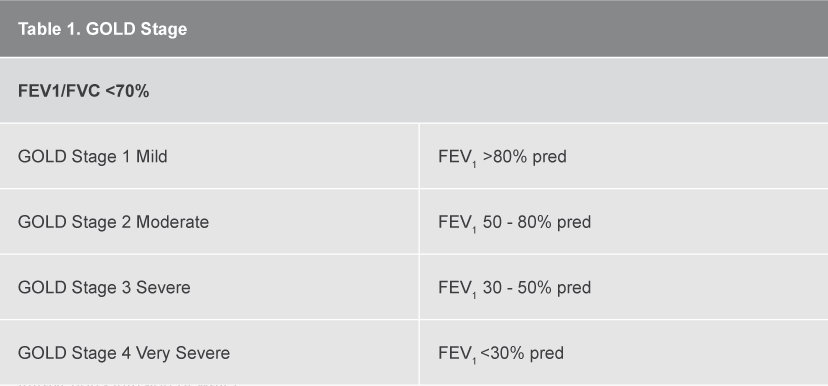
Table 1. Gold Stage
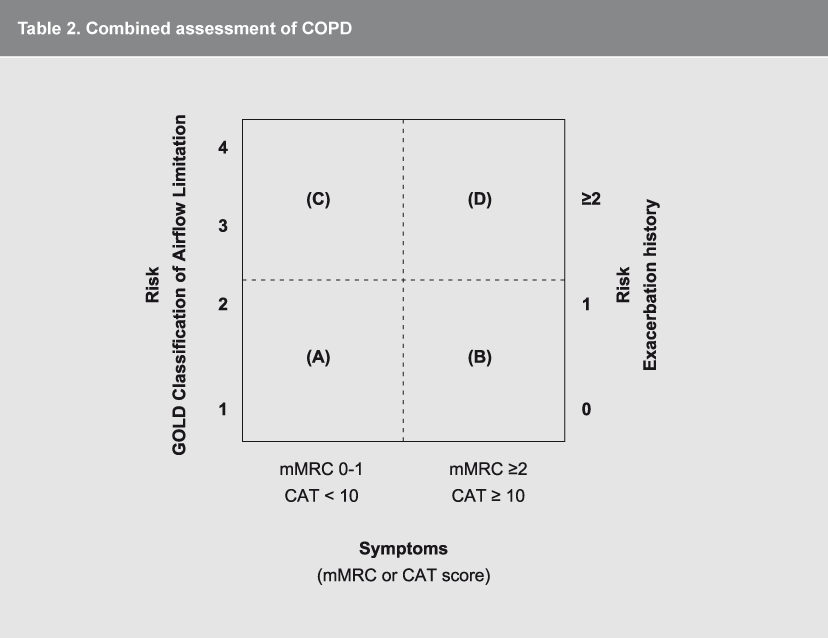
Table 2. Combined assessment of COPD

Table 3. mMRC Dyspnoea Score
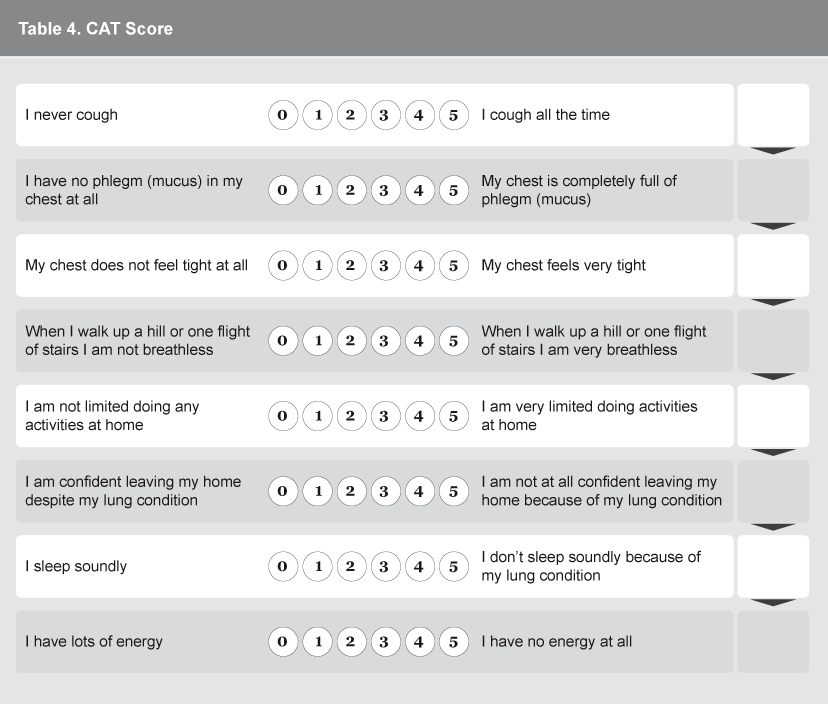
Table 4. CAT Score

Table 5. Exacerbation Frequency
Treatment Episode 1 – Time 0
The GP informs the patient of the diagnosis and provides him with written literature on COPD. She explains carefully that the disease is largely due to smoking and there may have been some contribution from his dusty job. She ascertains that the patient has been considering quitting smoking for some time. As the patient is in group D, she prescribes a long-acting anti-muscarinic inhaler and a twice daily inhaled corticosteroid/long-acting beta-2-agonist combination inhaler with salbutamol 1-2 puffs as needed. The practice nurse teaches correct inhaler technique. The GP also encourages the patient to walk at least 30 minutes daily and arranges to see the patient again in 4 weeks and orders a chest x-ray.
Treatment Episode 2 – 4 weeks later
The patient is very keen to quit smoking and agrees to take a 12 week course of varenicline. He is less breathless and has been walking more but still has to stop at 200m. He has had no further infections. He agrees to referral to the local hospital for pulmonary rehabilitation. He also agrees to receive pneumovax and the flu vaccination in early October 2013. Chest x-ray was reported as hyperinflated and the GP arranges a 3 month review.
Treatment Episode 3 – 3 months later
The patient has quit smoking for the last 10 weeks and has gained 4 kg in weight. He has had no further exacerbations. He has completed 4 sessions of pulmonary rehabilitation but feels his exercise tolerance is not improving. The GP explains that the weight he has gained after stopping smoking has balanced out the benefit so far from rehab and refers him to a dietitian. She also administers the flu vaccination. She arranges a 4 month review.
Treatment Episode 4 – 4 months later
The patient has remained off cigarettes and has managed to lose 12kg and has a BMI of 31. He attended all the rehab sessions and can now walk 800m without stopping. He has had 1 infective exacerbation of COPD over the winter and took 1 week of amoxicillin 500mg tds and prednisolone 30mg daily. He took about 3 weeks to fully recover from this exacerbation. The GP prescribes a home pack of the same treatment for emergency use.
References Text
- National Clinical Guideline Centre. (2010) COPD in adults in primary and secondary care. London: National Clinical Guideline Centre http://guidance.nice.org.uk/CG101/Guidance/pdf/English Last accessed June 2013.
- Global Strategy for the Diagnosis, Management and Prevention of COPD, Global Initiative for GOLD 2013. Available fromhttp://www.goldcopd.org. Last accessed June 2013.
- An official American Thoracic Society / European Respiratory Society statement: key concepts and advances in pulmonary rehabilitation. Spruit MA, et al. Am J Respir Crit Care Med. 2013;188(8):e13-64
- International variation in the prevalence of COPD (the BOLD Study): a population based prevalence study. Buist AS et al,Lancet 2007 ;370:741-50
- Salmeterol and fluticasone propionate and survival in COPD. Calverley PM et al, NEJM 2007;356:775-89
- Effect of Tiotropium on outcomes in patients with moderate COPD (UPLIFT): a pre-specified subgroup analysis of a randomised control trial. Lancet 2009;374(9696): 1171-8
- Susceptibility to exacerbation in COPD. Hurst JR et al,NEJM 2010;363:1128-38
- COPD exacerbations.2: aetiology. Sapey et al, Thorax 2006;61:250–258
- Once-daily bronchodilators for COPD: indacterol versus tiotropium. Am J Respir Crit Care Med 2010;182:155-62
- Analysis of COPD exacerbations with the dual bronchodilator QVA 149 compared with glycopyrronium and tiotropium (SPARK): a randomised double-blind, parallel-group study. Wedzicha et al, Lancet Respir Med. 2013;1:199-209.
